Anti-inflammatory diets have been around for some time. There are many websites, books and blogs promoting the benefits of eating anti-inflammatory foods.
This type of diet sounds tempting, not only because of the foods they promote – which are all delicious – but because the idea that we can fight inflammation with the foods we eat sounds so attractive and natural!
So what is an anti-inflammatory diet, what are they supposed to do and what’s the evidence (if any) behind them?
First – the what
The theory behind these diets is that certain foods have anti-inflammatory properties, while others cause inflammation. So if we incorporate more of the anti-inflammatory foods and less of the pro-inflammatory foods in our diets, it may help lower levels of inflammation for people who have arthritis, psoriasis and other inflammatory conditions.
Sounds logical, right? Maybe??
Next – the evidence
OK, so this is where it gets a little murky. There’s really not a lot of conclusive evidence to support these claims. Studying the effects of diet is a tricky business, as this article in VOX explains. When we look at treating chronic diseases, research “involves looking holistically at diets and other lifestyle behaviors, trying to tease out the risk factors that lead to illness. Nutrition science [is therefore] a lot more imprecise. It’s filled with contradictory studies that are each rife with flaws and limitations. The messiness of this field is a big reason why nutrition advice can be confusing.” (1)
So we often have to use things like observational studies, self-reporting or information gleaned from studying the effects of dietary changes on lab animals.
Which means the data we obtain is often contradictory and isn’t conclusive. For more information read: The messy facts about diet and inflammation by Scientific American.
Does this matter?
Maybe not. Two popular anti-inflammatory diets are the Mediterranean diet and the DASH (Dietary Approaches to Stop Hypertension) diet.
Both diets have a heavy emphasis on eating:
- foods that are as unprocessed as possible,
- a rainbow of fresh whole fruits and vegetables (not juices),
- whole grains such as brown rice, quinoa, oats, whole grain breads and pasta,
- beans, lentils, chick peas and other legumes,
- nuts and seeds,
- fish, seafood and poultry,
- healthy oils such as olive, vegetable, canola.
They both recommend people eat less:
- red meat,
- foods high in sugar, salt and fat,
- highly processed foods.
So if we look at this type of diet, it’s actually a healthy, well-balanced diet. Eating a variety of different foods, in a range of different colours means that we’re giving our body a wide range of important vitamins and nutrients.
In the end, whether you call it an anti-inflammatory diet, a Mediterranean diet or DASH diet, it doesn’t really matter. And whether it has an effect on inflammation, only time and further research will tell.
But if you eat a nutritious, well-balanced diet you’ll certainly feel better overall. Eating well helps us maintain a healthy weight, is important for our physical and mental health, can help us sleep better, be more active, reduce our risk of developing other health conditions, and just generally makes us feel good.
Tips to change your diet
If you want to make your diet more like the anti-inflammatory style of diet, here are our top tips:
- Talk with your doctor and seek advice from an accredited practising dietitian.
- Start small. You don’t have to change your entire diet at once if that seems overwhelming. Make small changes such as reducing the amount of processed foods you eat, eating more fruits and vegies each day, swap red meat for fish, lean chicken (skin-off), beans or lentils.
- Get adventurous. There are a lot of websites that provide easy recipes that follow this type of eating plan. We’ve listed some in the More to Explore section.
- Portion size is still important. Many of the plates we use, especially for dinner, are far too big. And we tend to fill them. The simple solution is to use a smaller plate. When dishing up your meals, imagine your plate is divided into quarters. Aim to fill two of those quarters (or half the plate) with colourful vegies or salad, one quarter with protein (fish, legumes, tofu, meat) and the last quarter with carbohydrate foods such as rice, noodles, potato or bread roll.
- Exercise is also important. A healthy diet doesn’t work on its own. We also need to be active every day to maintain our weight, control our pain, improve our sleep and improve our mood and mental health.
- Reduce your intake of:
o Sweet foods such as cakes and biscuits. Swap them for fresh, in-season fruit.
o Refined grains such as white rice and white bread. Swap them for whole grains.
o Trans-fats and saturated fats.
o Ultra-processed foods. These are foods that have gone through a LOT of processing and are far from their original state. They generally have salt, sugar, fat, additives, preservatives and/or artificial colours added.
Final words
At the end of the day, these diets are all about eating a variety of healthy foods. And as we come into warmer weather, these are the sorts of foods that make us happy, feel lighter and more energetic. So – if you’re not already – why not give it a go?
Call our Help Line
If you have questions about things like managing your pain, COVID-19, your musculoskeletal condition, treatment options, telehealth, or accessing services be sure to call our nurses. They’re available weekdays between 9am-5pm on 1800 263 265; email (helpline@muscha.org) or via Messenger.
More to explore
- Find an Accredited Practising Dietitian
Dietitians Australia - Anti-inflammatory diet do’s and don’ts
Arthritis Foundation (USA) - Health effects of a low-inflammatory diet in adults with arthritis: a systematic review and meta-analysis
Journal of Nutritional Science, 2020 - How can changing my diet help my arthritis?
Versus Arthritis (UK) - Mediterranean diet recipes
Taste.com.au - The Mediterranean diet
Queensland Health - The messy facts about diet and inflammation
Scientific American, 2018 - What’s the DASH diet?
Sanitarium
Reference
(1) I asked 8 researchers why the science of nutrition is so messy. Here’s what they said.
Vox, 2016






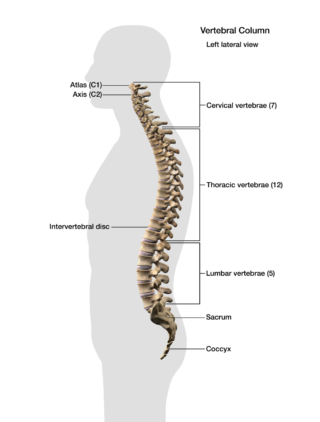 Let’s start with a look at your spine
Let’s start with a look at your spine











