It’s definitely a mouthful, but what is axial spondyloarthritis?
Axial spondyloarthritis (axSpA) is the umbrella term for two different types of inflammatory arthritis that affect the spine: ankylosing spondylitis (AS) and non-radiographic axial spondyloarthritis (nr-axSpA)
Ankylosing spondylitis (AS) affects the spine and the joints that connect the lower spine to the pelvis (sacroiliac joints). These changes are visible on x-ray.
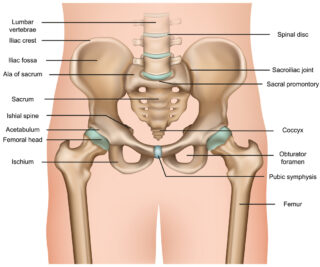
In non-radiographic axial spondyloarthritis (nr-axSpA), these changes aren’t yet visible on an x-ray but may be seen on an MRI. For some people, nr-axSpA will never progress to the stage where joint changes are seen on x-ray. For others, these changes will eventually be seen on an x-ray, and their diagnosis will be changed to AS.
These conditions cause pain, stiffness and reduced mobility in your spine. They can also cause symptoms including inflammation of tendons and ligaments, inflammatory bowel disease, psoriasis and inflammation of the eye.
The good news is that axSpA can be treated effectively with medicine and self-care.
Q. What are the signs that I may have axial spondyloarthritis?
A. The signs or symptoms of axial spondyloarthritis vary from person to person. The most common symptoms are pain and stiffness in the back, often the lower back and into the buttocks that:
- comes on gradually over weeks or months
- is worse in the second half of the night and wakes you up
- is worse first thing in the morning, with early morning stiffness that lasts 30 minutes or more
- is worse after rest and feels better after activity and exercise
- has been present for 3 months or more
- may involve pain deep in the buttock that can swap from one side to the other over time, especially in the early stages (doctors call this ‘alternating buttock pain’).
Other symptoms can include:
- fatigue (extreme tiredness)
- inflammation and pain in tendons (which connect muscles to bones) and ligaments (which connect bones to each other), which you may feel as pain in the front of your chest, back of your heel or underneath your foot
- arthritis in one or more of your peripheral joints – such as the joints in your hands, feet, arms or legs
- inflammation in your eye (uveitis)
- inflammatory bowel disease
- psoriasis
- feeling feverish and having night sweats
- losing your appetite and losing weight.
Symptoms may change from day to day. At times your symptoms (e.g. pain, fatigue, inflammation) can become more intense. This is a flare. Flares are unpredictable and can seem to come out of nowhere.
Q. What causes axial spondyloarthritis?
A. Axial spondyloarthritis is an autoimmune disease. That means it occurs as a result of a faulty immune system.
Instead of identifying foreign bodies (e.g. bacteria, viruses) and attacking them to keep you healthy, your immune system mistakenly targets healthy tissue in and around your joints, causing inflammation and pain.
We don’t know why this happens. Genes are thought to play a role. You’re more likely to get axSpA if you have a history of it in your family. Most people with axSpA have the gene called HLA-B27; however, this gene can also be found in people who don’t have axSpA.
Since this gene doesn’t automatically lead to the development of axSpA, other factors are thought to be involved.
We used to think axSpA affected more men than women, but recent research suggests men and women are affected relatively equally.
Q. How do I know if I have axial spondyloarthritis?
A. If you have ongoing back pain and stiffness or other symptoms of axSpA, it’s essential that you see your GP. Getting a diagnosis as soon as possible means that treatment can start quickly. This will give you the best possible outcomes.
No one test can diagnose axSpA, so your doctor will use a combination of tests to confirm your diagnosis. They may include:
- Your medical history. Your doctor will ask about your symptoms, family history and other health issues.
- A physical examination to assess joint tenderness, flexibility, and stiffness.
- Blood tests to check for inflammation associated with axSpA.
- Genetic testing to look for the HLA-B27 gene, which is present in most people with axSpA.
- Scans such as an x-ray and MRI (magnetic resonance imaging) to look for joint inflammation and damage.
Your GP will refer you to a rheumatologist if they think you have, or have diagnosed you with axSpA. Rheumatologists are doctors who specialise in diagnosing and treating problems with joints, muscles, bones and the immune system.
Q. How is axial spondyloarthritis treated?
A. Your rheumatologist will recommend and prescribe medicines for your axSpA.
The two main types of medicines used to treat axSpA and help manage its symptoms are NSAIDs and targeted therapies:
- Non-steroidal anti-inflammatory drugs (NSAIDs) are nearly always used as the first medicine to treat the pain, inflammation and stiffness of axSpA unless there’s a reason that you can’t take them. Research shows that NSAIDs are very effective in managing symptoms of axSpA. Some people may need to take them regularly, while others will only take them as needed. This will depend on your symptoms and how you respond to the NSAID. Your rheumatologist will talk with you about how often you should take NSAIDs and the long-term benefits and risks of using them. There are many different types and brands; some are available over-the-counter, while others are only available on prescription.
- Targeted therapies are medicines that ‘target’ specific proteins in the immune system that produce inflammation. They include biological disease-modifying anti-rheumatic drugs (biologics), biosimilars and targeted synthetic disease-modifying anti-rheumatic drugs. These targeted treatments have dramatically improved the quality of life for people with axSpA who need more than NSAIDs to manage their condition. They work to control your immune system in a targeted way, slowing down the attack on your spine and joints. Your rheumatologist will talk to you about using these medicines if you need more than NSAIDs to manage your axSpA or you’re unable to take NSAIDs.
Q. What can I do to control my symptoms?
A. As well as taking your medicines as prescribed, there are things you can do.
- Learn about your condition. Understanding axSpA allows you to make informed decisions about your healthcare and actively manage it.
- Exercise regularly. This is the most important thing you can do to help manage your axSpA. Exercise can improve symptoms including stiffness, pain, fatigue, breathing capacity and posture. It helps increase your flexibility and range of movement, so it’s easier to do many everyday tasks. As soon as possible after receiving your diagnosis, you should ideally begin a personalised exercise program developed by a physio or exercise physiologist (EP) and aim to do some exercise every day. Being active is also essential for your overall health and wellbeing. It helps keep your muscles, bones and joints strong so that you can keep moving. It reduces your risk of developing other conditions such as heart disease, osteoporosis, diabetes and some forms of cancer. It boosts your mood, benefits your mental health, helps with weight control and improves sleep.
- Manage your weight. Being overweight or obese increases inflammation throughout your body. This inflammation affects not only your joints but also blood vessels and insulin levels. This can increase your risk of chronic health conditions such as heart disease and diabetes. Losing weight is an important thing you can do to reduce your risk of these conditions and to reduce your axSpA symptoms. Being overweight or obese also limits the effectiveness of some medicines used to treat axSpA. Losing weight can be challenging, so if you need to lose weight or advice on healthy eating, talk with your doctor or dietitian.
- Learn ways to manage your pain. Pain is the most common symptom of axSpA, so learning to manage it effectively is crucial. Read our A-Z guide for managing pain for more information.
- Work closely with your healthcare team. The best way to live well with axSpA is by working closely with the people in your healthcare team (e.g. GP, rheumatologist, physio). Keep them informed about how you’re doing and if you’ve experienced any changes in your symptoms or tried new medicines, complementary therapies, supplements or other treatments.
- Use aids and equipment. Supports such as long-handled shoehorns, reachers and canes can reduce joint strain and make life easier, especially if your condition has reduced your flexibility and mobility. An occupational therapist can advise you on aids, equipment and home modifications. You can also check out our range of aids in our online shop.
- Sleep well. Not getting enough quality sleep can worsen your symptoms; however, getting a good night’s sleep when you have axSpA and chronic pain can be difficult. If you’re having problems sleeping, talk with your doctor about ways you can address this.
- Manage stress. Stress can also aggravate your symptoms, so learning to deal with stress is extremely helpful. Things you can do to manage stress include planning your day and setting priorities, using relaxation techniques such as going for a walk, getting a massage or listening to music, and, where possible, avoiding people and situations that cause you stress.
- Practise mindfulness. Regularly practising mindfulness meditation can improve your mood, relieve stress, improve sleep, improve mental health and reduce pain.
- Eat a healthy, balanced diet. While there’s no specific diet for axSpA, it’s important to have a healthy, balanced diet to maintain general health and prevent weight gain and other health problems, such as diabetes and heart disease.
- Quit smoking. Smoking cigarettes is not only bad for your general health but also negatively affects your bone health and increases inflammation.
- Seek support from others. You might find it helpful to contact Ankylosing Spondylitis Australia or the Ankylosing Spondylitis Group of Victoria and speak to others who have axSpA and know what you’re going through.
Q. Are there any complications I should be aware of?
A. Some people living with axSpA develop an eye problem called uveitis, which causes a painful red eye with blurred vision and sensitivity to light.
If you develop eye symptoms, you’ll need to quickly get your eye checked and treated by an ophthalmologist. Treatment is usually with prescription eye drops, which reduce the chance of permanent eye damage.
By understanding this risk and knowing what signs to be alert for, you can reduce the risk of damage to your eyes.
Ask your GP or rheumatologist what you should do if you develop any eye symptoms.
Q. What about surgery?
A. Most people with axSpA can manage their condition using a combination of exercise, medicines and self-care.
However, surgery may be considered in some cases if treatments haven’t provided relief from symptoms or if you have a spinal fracture or dislocation. Surgery that may be considered includes:
- hip arthroplasty (replacement) surgery if you have severe and persistent hip pain
- cervical fusion, where bones in the cervical (upper) spine are fused together to treat a fracture or dislocation
- wedge osteotomy removes a wedge-shaped piece of bone from a vertebra to allow the spine to be realigned.
If your doctor thinks surgery might be an option, they’ll refer you to an orthopaedic surgeon. Together, you can discuss the benefits and risks of surgery and decide if it’s right for you. If you’re unsure about surgery or don’t feel comfortable with the information from the surgeon, ask your doctor to refer you to another surgeon for a second opinion.
Contact our free national Help Line
Call our nurses if you have questions about managing your pain, musculoskeletal condition, treatment options, mental health issues, COVID-19, telehealth, or accessing services. They’re available weekdays between 9am-5pm on 1800 263 265; email (helpline@msk.org.au) or via Messenger.
More to explore
- About the disease
Spondylitis Association of America - Ankylosing spondylitis
Versus Arthritis UK - Axial spondyloarthritis
Arthritis Foundation - Back Yourself – ankylosing spondylitis patient empowerment website
Abbvie - Patient education: Axial spondyloarthritis, including ankylosing spondylitis (Beyond the Basics)
UpToDate - What is axial SpA?
National Axial Spondyloarthritis Society